Grade 3 Hemorrhoids: When to See a Doctor
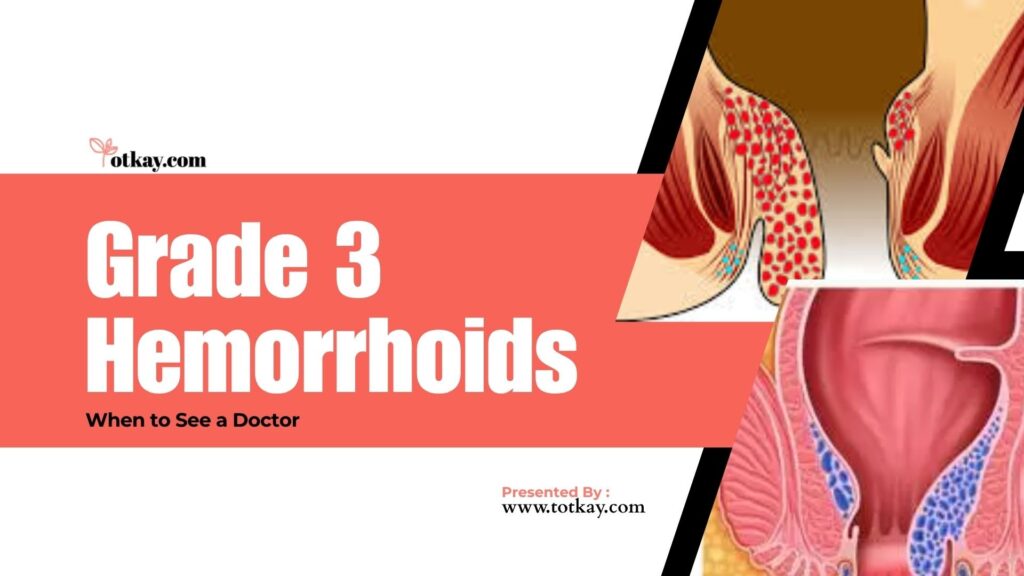
Grade 3 Hemorrhoids occur when prolapsed anal tissue comes out during bowel movements and must be pushed back manually. At this stage, patients often experience a painful bowel movement, swelling outside anus, and recurring discomfort throughout the day.
Unlike earlier stages, this condition signals a higher risk of hemorrhoid complications, including clot formation and infection. While temporary relief is possible, most individuals require a doctor consultation piles to prevent worsening and avoid progression to more severe stages.
Scenario First: “You Feel a Lump That Won’t Go Back”
This is how most people first realize something is wrong. You finish your bathroom routine and notice a distinct change. Something feels stuck outside, and it does not go back on its own.
This defining moment separates early-stage issues from advanced Grade 3 Hemorrhoids. Patients typically observe the following reality:
- The tissue remains outside the body after a bowel movement.
- You must use your fingers to manually push the lump back inside.
- The area feels tender, swollen, and highly sensitive to touch.
What’s Actually Happening Inside Your Body
Understanding reduces fear and confusion. Internal changes cause the physical symptoms you experience. The vascular structures in your lower rectum undergo significant physical stress.
It is not just swelling; it is a structural change. Consider these internal developments:
- Severely Swollen Veins: The veins in your lower rectum become so swollen that they are now permanently enlarged.
- Weakened Supportive Tissues: The tissues that are supposed to hold these veins in place have lost their strength and elasticity.
- Constant Prolapse: Because the veins are enlarged and the tissues are weak, the prolapse happens regularly and is no longer just an occasional event.
The “Push-Back” Stage: Why This Is a Serious Turning Point
Manual repositioning is not normal. When your body cannot self-correct, the condition is progressing. This mechanical failure indicates that the structural integrity of the anal canal is compromised.
This is where self-care stops being enough. The physical act of pushing tissue back indicates severe internal weakness:
- Loss of Internal Support: The ligaments meant to anchor your internal tissues are failing. They can no longer support the vascular cushions, leading to prolapse.
- Risk of Injury: Each time you manually push the tissue back, the friction can cause small tears (micro-tears), worsening the irritation and potential for bleeding.
- Increased Infection Risk: The repeated physical handling introduces external bacteria to a sensitive internal area, making infections more likely.
Daily Life Impact: What Changes at Grade 3
This stage affects routine activities. You start planning your day around your bathroom habits. A simple office job or a long commute suddenly turns into a painful challenge.
It becomes a lifestyle problem, not just a symptom. You will likely experience a severe disruption in everyday comfort:
- Prolonged Sitting Becomes Unbearable: Even simple tasks like working at a desk for extended periods cause significant discomfort and pain.
- Anxiety Around Bowel Movements: The anticipation of pain turns every trip to the bathroom into a source of fear and anxiety.
- Constant Physical Discomfort: A persistent awareness of the external swelling becomes a constant, distracting irritation throughout your day.
- Difficulty with Physical Activities: Exercise, lifting heavy objects, or even vigorous walking can worsen the swelling and discomfort, limiting your active lifestyle.
- Social and Professional Life Suffers: The need for frequent, long bathroom breaks and the inability to sit comfortably can lead to avoiding social events or struggling to perform at work.
- Hygiene Challenges: Keeping the area clean becomes more difficult due to the external tissue, increasing the risk of irritation and secondary infections.
Silent Warning Signs Most People Ignore

Not all danger signs are obvious. Many individuals adapt to the discomfort and ignore the subtle shifts in their symptoms. Ignoring these shifts allows the condition to deteriorate quietly.
These are early signals of hemorrhoid complications. Watch closely for these hidden indicators of disease progression:
- You find yourself needing to push the tissue back repeatedly throughout the day.
- The swelling lasts much longer after leaving the toilet than it did previously.
- The base level of pain increases gradually over several weeks.
The Risk Zone: When Grade 3 Becomes Dangerous
Some symptoms should never be ignored. When vascular tissue remains outside the body, the blood supply can become compromised. A sudden shift in your symptoms requires immediate medical evaluation.
This may indicate thrombosed hemorrhoids or tissue strangulation. Seek urgent care if you experience any of the following severe symptoms:
Severe, Stabbing Pain
If you experience a sudden, sharp, or stabbing pain, it could signal a thrombosed hemorrhoid. This happens when a blood clot forms within the hemorrhoid, leading to intense discomfort and swelling. Don’t try to wait this out; the pain is a clear warning sign that requires immediate medical attention to prevent further complications.
Dark or Continuous Rectal Bleeding
While minor bleeding can be common with hemorrhoids, dark or excessive bleeding is not. Continuous bleeding or the passing of dark, tarry stools indicates a more serious issue that needs urgent evaluation. This type of bleeding could point to significant blood loss or other internal problems that a doctor must assess right away.
A Hard, Irreducible Lump
If a prolapsed hemorrhoid becomes hard and you can’t gently push it back inside, it may be strangulated, meaning its blood supply is cut off. This is a medical emergency that can lead to tissue death (necrosis) if not treated promptly. Feel for a firm, tender lump at the anal verge that was previously soft or reducible.
The Decision Framework: Should You See a Doctor Now?
This removes confusion completely. Knowing exactly when to seek professional help saves you from unnecessary suffering. Use this clear framework to determine your next exact steps.
Waiting usually makes the medical intervention more complex. Evaluate your current situation against these clear clinical markers:
| Situation You Face | What It Means | What You Should Do |
| must push hemorrhoid back daily | confirmed Grade 3 | schedule doctor visit |
| pain increasing over time | worsening condition | consult urgently |
| bleeding frequently | tissue damage | medical evaluation needed |
| swelling stays outside longer | risk of progression | do not delay treatment |
Why Home Remedies Stop Working at This Stage
Many people rely on wrong solutions. Over-the-counter treatments target mild surface inflammation, not structural collapse. Applying topical ointments to a mechanical prolapse provides zero long-term benefit.
These manage symptoms, not the condition itself. Relying on conservative treatments at this stage only delays inevitable medical care:
- Topical Creams: These might soothe surface irritation for a little while, but they can’t fix the underlying structural problem.
- Warm Sitz Baths: While they feel good and offer temporary relief, they don’t have the power to restore the tissue’s original strength and position.
- Dietary Fiber: Eating more fiber is great for softening your stool, which prevents further strain, but it can’t undo a prolapse that has already occurred.
What Doctors Actually Do (Reality Check)
Treatment is simpler than people fear. Medical advancements have made piles treatment highly efficient. Most interventions occur right in the doctor’s office without the need for hospital admission.
An early visit means you qualify for a less invasive treatment plan. Medical professionals utilize several precise approaches to resolve the issue:
Office-Based Procedures
Doctors perform these quick, non-surgical treatments in minutes. They require minimal recovery time and allow you to return to work quickly.
Minimally Invasive Options
These specialized techniques shrink or remove the problematic tissue safely. They target the blood supply of the enlarged vein to cause it to wither and fall off.
Surgery (Only If Needed)
Surgeons reserve full operative hemorrhoidectomies for severe or long-term cases. This option provides a permanent fix when less invasive methods cannot resolve the large tissue mass.
What Happens If You Wait Too Long
Delay has real consequences. The supportive tissues will continue to stretch until they break down completely. Once the tissue permanently prolapses, your treatment options narrow significantly.
Waiting increases both your daily pain and your overall medical costs. Refusing to seek treatment leads to severe physical outcomes:
- Permanent Prolapse (Grade 4): The tissue will prolapse permanently and cannot be manually pushed back in.
- Severe Complications: Your risk of intense pain, bleeding, and dangerous blood clots increases significantly.
- Invasive Surgery: You will have no choice but to undergo extensive and painful surgery as your only remaining treatment option.
Final Thoughts
Grade 3 Hemorrhoids represent a critical juncture in your physical health. When you constantly deal with prolapsed anal tissue, you risk severe and painful hemorrhoid complications. Ignoring the mechanical failure of your internal tissues will only lead to more invasive surgical requirements down the road.
Do not let embarrassment or fear delay your healing process. A timely doctor consultation piles provides clarity, professional guidance, and fast relief from the daily disruption. Take control of your health today by scheduling an appointment with a gastroenterologist or colorectal specialist to discuss your targeted treatment options.
For more in-depth information on managing piles and to explore our guides on Grade 1 and Grade 2 hemorrhoids, visit totkay.com—your trusted resource for expert health content.
Frequently Asked Questions
What makes Grade 3 hemorrhoids different from other stages?
Grade 3 hemorrhoids are distinct because the prolapsed tissue requires manual repositioning. Unlike earlier grades where it either remains inside or retracts on its own, this stage requires intervention.
Can Grade 3 hemorrhoids be treated at home?
While home remedies like sitz baths and high-fiber diets can alleviate symptoms, they cannot resolve the underlying prolapse. Professional medical treatment is necessary to address the mechanical issue effectively.
Is surgery the only option for Grade 3 hemorrhoids?
No, surgery is not the only option. Minimally invasive procedures like rubber band ligation or sclerotherapy are often effective for Grade 3 hemorrhoids and are less invasive than a traditional hemorrhoidectomy.
What happens if Grade 3 hemorrhoids are left untreated?
Ignoring Grade 3 hemorrhoids can lead to serious complications, including thrombosis (blood clots), severe pain, and the progression to Grade 4, where the prolapse cannot be pushed back in.
Why do I have to push my hemorrhoids back in?
The need to manually push back prolapsed tissue indicates that the supportive structures within the anal canal have weakened significantly. This is a clear sign of an advanced hemorrhoid stage.
When should I see a doctor for Grade 3 hemorrhoids?
You should see a doctor immediately if you need to manually reposition hemorrhoids. Prompt medical evaluation can prevent further complications and provide access to effective, minimally invasive treatment options.

Hi, I’m a dedicated writer at Totkay.com, passionate about sharing practical tips and solutions to make your life easier. Explore my articles for helpful insights and valuable advice. Stay connected for more expert content!






