What Are Piles? Causes, Symptoms & Treatment

Many people experience bleeding during stool or anal discomfort at some point in their lives. Most stay silent about it, assuming it will resolve on its own. That silence can delay treatment and allow a manageable condition to worsen.
Piles are swollen veins in the anus or lower rectum. Studies estimate that hemorrhoids affect around 10–15% of adults worldwide, making them one of the most common anorectal disorders. Yet, because of the stigma surrounding the topic, many people avoid seeking the help they need.
Piles develop when pressure builds up in the rectal veins, often due to constipation, prolonged sitting, or straining during bowel movements. The condition can cause pain, itching, and rectal bleeding — symptoms that significantly affect daily life when left unaddressed.
This article explains what piles are, what causes them, how to recognize the symptoms, and what treatment and prevention strategies are available.
What Are Piles?
Piles are inflamed or swollen blood vessels located in the anal canal. When pressure builds in the veins surrounding the rectum, those veins begin to stretch and swell — much like varicose veins in the legs, but occurring in the rectal area.
Medical literature describes hemorrhoids as vascular structures that become swollen due to increased venous pressure in the rectal area. This swelling can occur inside the rectum or outside the anus, and the location plays a large role in determining the symptoms a person experiences.
Types of Piles
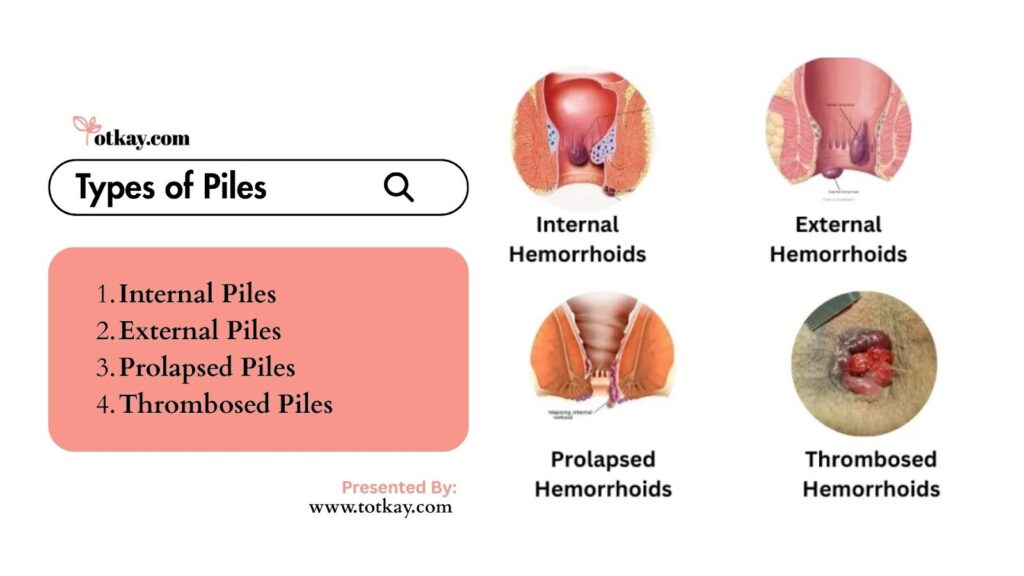
Piles are categorized based on their location and severity, which helps determine the most effective treatment. They can develop inside the rectum or under the skin around the anus, each presenting a unique set of symptoms.
Internal Piles
Internal piles develop inside the rectum and are often painless because there are fewer nerve endings in this area.
- Key symptom: The most common sign is bright red blood on toilet paper or in the toilet bowl during a bowel movement.
External Piles
External piles form under the skin around the anus, where there are more pain-sensing nerves. This makes them more symptomatic than internal piles.
- Key symptoms: They often cause noticeable pain, itching, swelling, and significant discomfort, particularly when sitting or passing stool.
Prolapsed Piles
Prolapsed piles are internal piles that have swollen and pushed through the anal opening. Their severity is graded based on how far they extend and whether they retract on their own.
- Key symptom: A noticeable lump or bulge extending from the anus, which may be accompanied by pain and bleeding.
Thrombosed Piles
A thrombosed pile occurs when a blood clot forms within an external or internal pile, blocking blood flow. This condition can be extremely painful and requires timely medical evaluation.
- Key symptoms: Sudden, severe rectal pain and a hard, tender lump near the anus.
Common Symptoms of Piles
Common symptoms include:
- Bleeding during bowel movements — bright red blood on stool or tissue
- Swollen veins around the anus — visible lumps or bulges near the anal opening
- Rectal pain or discomfort, particularly when sitting or passing stool
- Itching and irritation in and around the anal area
- A soft or hard lump near the anus
- Mucus discharge after a bowel movement
- Persistent discomfort while sitting for extended periods
Clinical studies confirm that the most common hemorrhoid symptoms are rectal bleeding, pain, and itching. If you experience any combination of the above, consult a healthcare professional.
Early Warning Signs of Piles
Piles rarely appear without warning. In most cases, the condition starts with subtle signs that are easy to dismiss. Catching these early can prevent the condition from progressing.
Early signs of Piles include:
- Slight itching or tingling in the anal area with no obvious cause
- Mild swelling near the anus after bowel movements
- Occasional spotting of blood during or after passing stool
- Irritation or a feeling of incomplete emptying after bowel movements
These early symptoms do not always indicate a severe problem, but they are a signal that pressure and inflammation are developing. Addressing the underlying causes at this stage — such as improving diet and hydration — can prevent more serious stages of the condition.
What Causes Piles?
Piles develop when pressure increases in the rectal veins over time. Several factors contribute to this pressure buildup. Here is what medical evidence points to as the primary causes.
- Chronic Constipation: causes of rectal painrectal pain causes. Hard stools force repeated pressure onto the veins in the anal canal, causing them to swell.
- Prolonged Sitting: Sitting for long periods reduces blood circulation in the anal region. This slows venous drainage and increases pressure in the rectal veins. Studies show that constipation and prolonged sitting are major risk factors for hemorrhoids.
- Low-Fiber Diet: A diet low in fiber produces hard, dry stools. These are difficult to pass and require greater straining, a direct contributor to piles.
- Pregnancy: During pregnancy, the growing uterus places additional pressure on the rectal veins. Hormonal changes also soften the walls of blood vessels, making them more susceptible to swelling.
- Obesity: Excess body weight increases pressure throughout the abdominal region, including the veins surrounding the rectum.
- Heavy Lifting: Repeated heavy lifting or physical exertion that causes straining elevates venous pressure in the rectal area and raises the risk of developing piles.
Risk Factors That Increase the Chances of Piles
Certain lifestyle and biological factors make some individuals more likely to develop piles than others. Are any of these factors present in your life? Being aware of them can help you make more informed health decisions.
Key risk factors include:
- A sedentary lifestyle with little regular movement
- Lack of physical activity or structured exercise
- Advancing age, as the tissue supporting the anal veins weakens over time
- A genetic predisposition to weak vein walls or connective tissue
- Chronic diarrhea, which irritates the anal lining through repeated inflammation
- Poor bowel habits, including holding in stools or excessive toilet time
Research indicates that sedentary behavior and lack of exercise significantly increase hemorrhoid risk. Many of these risk factors are modifiable, meaning lifestyle adjustments can reduce your likelihood of developing the condition.
Stages of Piles (Grades)
Piles are classified into four grades based on severity. This grading system helps doctors select the most appropriate treatment.
Understanding the stage of your hemorrhoids is crucial for effective treatment. Doctors categorize them into four grades, from mild internal swelling to severe, permanent prolapse. This classification helps determine the best course of action, whether it’s lifestyle changes, non-invasive procedures, or surgery.
Grade 1:
These are small, internal hemorrhoids that develop inside the rectum. They are not visible from the outside and typically don’t cause pain, though they might bleed. Because they don’t protrude, they are usually only discovered during a medical examination.
Grade 2:
Larger than Grade 1, these piles prolapse (slip outside the anus) during a bowel movement. However, they retract back inside on their own afterward. This stage can cause more noticeable symptoms like itching and bleeding.
Grade 3:
Similar to Grade 2, these hemorrhoids prolapse during bowel movements but do not return to their original position automatically. They must be manually pushed back inside the anus. This stage often involves more discomfort and a greater risk of complications.
Grade 4:
This is the most severe stage, where the hemorrhoid remains permanently prolapsed outside the anus and cannot be pushed back in. This grade can cause significant pain, discomfort, and potential complications like blood clots, often requiring surgical intervention.
How Doctors Diagnose Piles
A proper diagnosis is essential. Rectal bleeding can result from several conditions, and only a qualified doctor can confirm whether piles are the cause.
Doctors typically use one or more of the following methods:
- Physical examination: Visual inspection of the anal area for external swollen veins around the anus
- Digital rectal exam: The doctor inserts a gloved finger into the rectum to feel for abnormalities
- Anoscopy: A short, lighted tube is used to examine the inner lining of the anal canal
- Colonoscopy: Recommended in more severe cases to rule out other colorectal conditions, such as polyps or colorectal cancer
Seeking a diagnosis is especially important when bleeding is present, as this symptom can overlap with more serious digestive conditions.
How to Get Rid of Piles?
Home Remedies and Lifestyle Changes
Mild to moderate cases of piles often respond well to non-medical management. Studies show that increasing dietary fiber significantly reduces hemorrhoid symptoms. Practical steps include:
- Eating fiber-rich foods such as fruits, vegetables, legumes, and whole grains can help soften stools
- Drinking at least 8 glasses of water daily to promote regular, comfortable bowel movements
- Taking warm sitz baths for 15–20 minutes to reduce anal discomfort and swelling
- Engaging in regular physical exercise to improve circulation and digestive function
- Avoiding straining during bowel movements, which worsens venous pressure
Medications
When lifestyle changes alone are not sufficient, doctors may recommend:
- Topical creams or ointments to reduce itching, swelling, and anal discomfort
- Anti-inflammatory medications to control pain and inflammation in the rectal area
- Stool softeners to ease the passage of stools and reduce straining
Non-Surgical Treatments
For piles that do not respond to conservative management, outpatient procedures are available:
- Rubber band ligation: A small band is placed around the base of the pile to cut off its blood supply
- Sclerotherapy: A chemical solution is injected into the vein to shrink it
- Infrared coagulation: Heat is applied to the pile tissue to reduce blood flow and cause it to shrink
Natural Ways to Prevent Piles

Prevention is far more comfortable than treatment. Many cases of piles are avoidable with consistent healthy habits. What daily steps can you take to protect yourself?
Effective prevention strategies include:
- Eat a high-fiber diet: To keep stools soft and regular, aim to eat plenty of fruits, vegetables, and whole grains every day. This simple dietary change is one of the most effective ways to prevent straining.
- Stay well-hydrated: Drinking enough water throughout the day is crucial. Limit caffeine and alcohol, as they can lead to dehydration, which makes stools harder to pass.
- Exercise regularly: Consistent physical activity, even a brisk 30-minute walk, helps stimulate bowel function and improves overall circulation, reducing pressure on your veins.
- Avoid prolonged sitting: Sitting for long periods, especially on hard surfaces, increases pressure on the veins in the rectum. If you have a desk job, make sure to get up and move around frequently.
- Don’t delay bowel movements: When you feel the urge to go, go. Holding it in can cause stool to become harder and drier, leading to straining and increased pressure.
Modern Lifestyle Habits That Increase Piles Risk
Modern daily habits have quietly created ideal conditions for piles to develop. The following behaviors elevate risk:
- Desk jobs that involve sitting for 6–10 hours per day without movement breaks
- Low physical activity between work and home
- Spending excessive time sitting on the toilet, which places sustained downward pressure on anal veins
- Smartphone or tablet use in the bathroom, which prolongs toilet time significantly
Some studies show that prolonged toilet sitting increases pressure on rectal veins. Even small behavioral changes — standing up regularly at work, limiting phone use in the bathroom — can make a measurable difference over time.
When Should You See a Doctor?
Some pile symptoms warrant prompt medical attention. Do not delay in seeking help if you experience any of the following:
- Rectal bleeding that is heavy, frequent, or does not resolve within a few days
- Severe rectal pain that interferes with daily activities
- Symptoms that persist for several weeks despite home treatment
- Stool that appears black or tarry, which may indicate bleeding higher in the digestive tract
Black or tarry stools are not typical of piles and may signal a more serious gastrointestinal condition. In this case, seek medical attention immediately.
Take Control of Your Digestive Health
Piles are far more common than most people acknowledge, and far more treatable than many assume. The condition develops gradually, often starting with mild hemorrhoid symptoms such as occasional itching or bleeding during stool, and progressing only when the underlying causes go unaddressed.
Understanding the causes, recognizing the anal discomfort and other early warning signs, and taking action promptly — whether through lifestyle changes, medication, or medical procedures — gives you real control over your digestive health.
Do not let discomfort persist in silence. If you recognize the symptoms described in this article, consult a healthcare professional. Early intervention prevents complications and restores quality of life far more quickly than delayed treatment.
Frequently Asked Questions (FAQ)
Can piles go away on their own?
Mild cases of piles, particularly Grade 1 and Grade 2, can resolve with dietary and lifestyle improvements. Drinking more water, increasing fiber intake, and avoiding straining often bring noticeable relief within a few weeks.
Is bleeding during stool always caused by piles?
Not always. Bleeding during stool is a common sign of piles, but it can also indicate other conditions, including anal fissures, colorectal polyps, or colorectal cancer. Any rectal bleeding should be evaluated by a doctor, particularly if it is persistent, heavy, or accompanied by a change in bowel habits.
Can ajwain and khush podina ka kawa help with piles?
Yes, ajwain (carom seeds) and khush podina (mint) ka kawa is often used in traditional remedies to support digestion and reduce symptoms linked with piles. Ajwain helps improve digestion and reduce gas, while mint can soothe the digestive system and reduce inflammation. Together, they may help ease constipation, which is a common trigger for piles. However, this remedy supports symptom relief and is not a complete medical treatment.
What foods should you avoid with piles?
Avoid processed foods, refined carbohydrates, spicy foods, and alcohol, as these can worsen constipation and increase anal discomfort. Caffeine and dairy may also contribute to hard stools in some individuals.
Are piles dangerous?
In most cases, piles are not life-threatening. However, chronic, untreated piles can lead to anemia and significant discomfort. Thrombosed or strangulated hemorrhoids are medical emergencies that require immediate care.
How should ajwain and khush podina ka kawa be used for piles?
To prepare the kawa, boil about ½ teaspoon of ajwain and a small handful of fresh khush podina leaves in one cup of water for 5–7 minutes. Strain and drink it warm once or twice a day, preferably after meals. Consistency, along with a high-fiber diet and plenty of water, can help manage piles symptoms better. If symptoms are severe or persistent, it is best to consult a doctor.

Hi, I’m a dedicated writer at Totkay.com, passionate about sharing practical tips and solutions to make your life easier. Explore my articles for helpful insights and valuable advice. Stay connected for more expert content!






